Baseline predictors of pathological Q Waves and their associations with different angiographic findings in patients with ST- segment elevation myocardial infarction treated by primary percutaneous coronary intervention
ORIGINAL RESEARCH ARTICLE
Baseline predictors of pathological Q Waves and their associations with different angiographic findings in patients with ST- segment elevation myocardial infarction treated by primary percutaneous coronary intervention
Article Summary
- DOI: 10.24969/hvt.2025.557
- CARDIOVASCULAR DISEASES
- Published: 30/03/2025
- Received: 19/01/2025
- Revised: 27/02/2025
- Accepted: 27/02/2025
- Views: 9344
- Downloads: 2777
- Keywords: Electrocardiogram, Q wave, ST-elevation myocardial infarction, primary percutaneous coronary intervention, predictors, TIMI flow, coronary thrombus, time to intervention, logistic regression analysis, observational study
Address for Correspondence: Amr Youssef Hassan, Cardiovascular Medicine Department, Cairo University, Egypt, 27 Nafezet Sheem El Shafaey Street, Cairo, Egypt
Email: amryoussef@kasralainy.edu.eg Phone: +20 111 804 11 32
ORCID: 0000-0002-7621-4246
Amr Youssef Hassan*, Talaat Al Hachem, Mohamed Al Ramly, Hussien Heshmat Kassem
Cardiovascular Medicine Department, Cairo University, El Saray Street Manial, El Manial, Cairo, 11956 –Manial, Egypt
Abstract
Objective: Q waves on the electrocardiogram (ECG) of patients presenting with ST-segment elevation myocardial infarction (STEMI) was an independent predictor of adverse clinical outcomes.
Aim of the study was to determine baseline predictors in patients who are likely to develop Q waves and their association with different angiographic findings.
Methods: Standard 12-lead ECG was recorded in 262 STEMI patients treated with primary percutaneous coronary intervention (PCI). An ECG was scored as Q-wave MI according to the “classic” criteria. Demographic, clinical data, and different angiographic findings were recorded for patients who had primary PCI strategy.
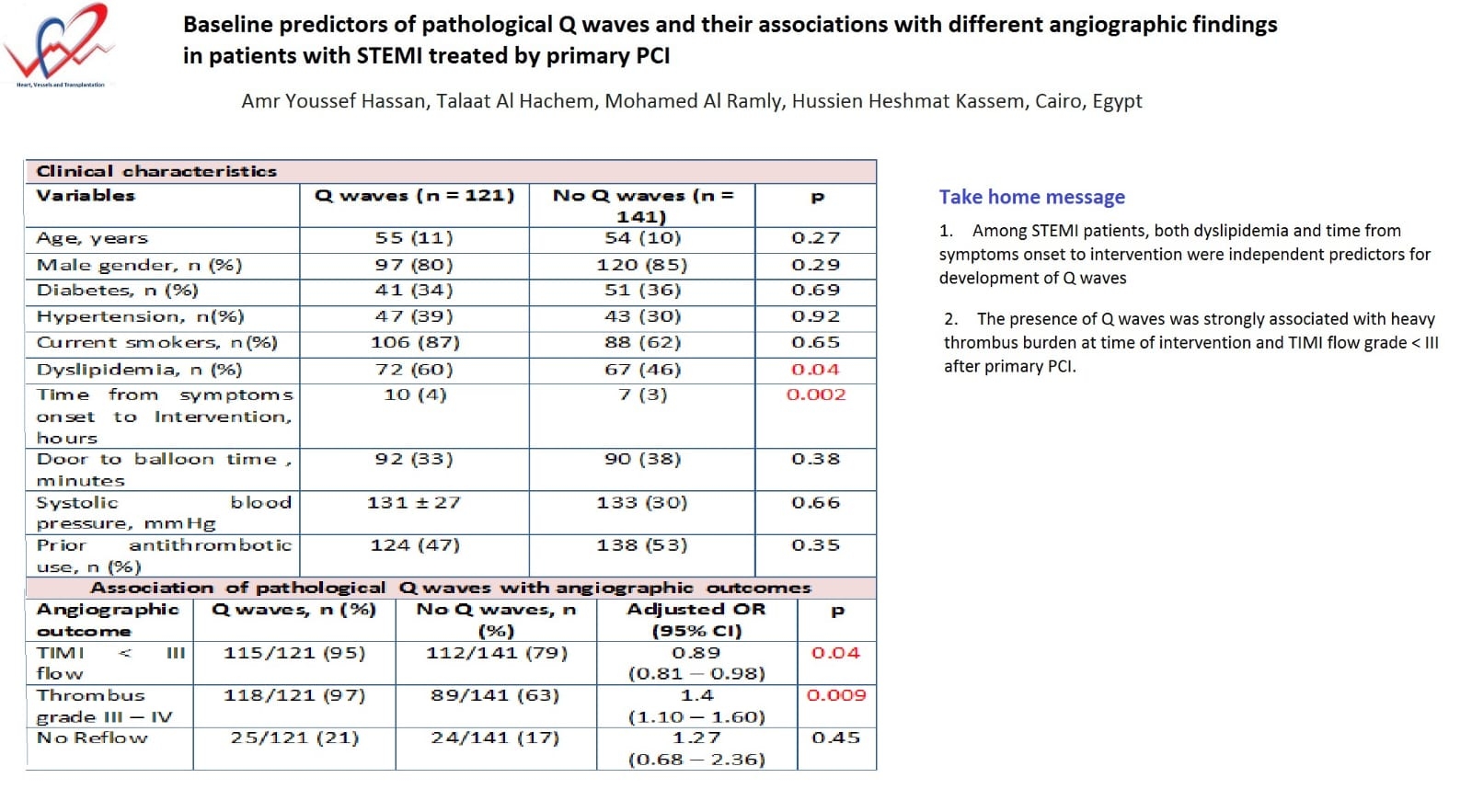
Results: Q waves were identified in 121 patients (46%). Both dyslipidemia and time from symptoms onset to intervention were independently and positively correlated with presence of Q wave (OR: 1.8, 95% CI 1.09 – 2.7, p = 0.04 for dyslipidemia), (OR: 1.35, 95%CI 1.09-1.67, p = 0.002 for time from symptoms onset). Patients with Q waves were more likely to have thrombus grade III - IV (OR: 1.4, 95% CI 1.10 – 1.60, p = 0.009) and TIMI flow grade < III (adjusted OR: 0.89, 95%CI 0.81 – 0.98, p=0.04). Dyslipidemia was an independent predictor for no reflow (p= 0.03). Diabetes and time from symptoms onset were independent predictors for thrombus grade III-IV (p = 0.007 and p=0.003 respectively).
Conclusion: Among STEMI patients, both dyslipidemia and time from symptoms onset to intervention were independent predictors for development of Q waves. The presence of Q waves was strongly associated with heavy thrombus burden at time of intervention and TIMI flow grade < III after primary PCI.
Key words: Electrocardiogram, Q wave, ST-elevation myocardial infarction, primary percutaneous coronary intervention, predictors, TIMI flow, coronary thrombus, time to intervention, logistic regression analysis, observational study
Introduction
The electrocardiogram (ECG) plays an integral role in the diagnosis of myocardial infarction (MI), due to universal availability and low costs. Patients are stratified in the acute coronary syndrome setting into ST-segment elevation myocardial infarction (STEMI) or non–ST segment elevation myocardial infarction based on presenting ECG. Pathological Q waves may develop after acute setting and were considered as classic ECG sign of necrosis (area of myocardium that cannot be depolarized) (1).
Over the years, there have been several definitions of Q waves. Earlier, pathological Q-wave was defined as wave with more than 0.04 sec of duration and with an amplitude of more than 25% of the corresponding R-wave (2-4). Consensus documents in 2007 redefined the ECG criteria again: (1) Any Q-wave in leads V2 –V3 ≥ 20 msec or QS complex in leads V2 and V3 (2); Q-wave ≥30 msec and ≥0.1 mV deep or QS complex in leads I, II, aVL, aVF or V4 –V6 in any 2 leads of a contiguous lead grouping (I, aVL, V 6; V 4 –V 6; II, III, and aVF)
(3) R-wave ≥40 msec in V1 –V2 and R/S ≥1 with a concordant positive T-wave in the absence of a conduction defect (5).
Q waves on the (ECG) of patients presenting with STEMI was an independent predictor of adverse clinical outcomes (6-8). However, there is a limited evidence about association of pathological Q wave in patients with MI and different angiographic outcomes. In addition, baseline predictors in patients who likely develop Q waves are incompletely defined.
The aims of this study were to identify predictors of Q-wave development among patients undergoing primary PCI due to STEMI and assess whether there is an association between development of Q waves on ECG and different angiographic findings during primary PCI procedure.
Methods
Study design and population
This was a prospective, historical, single center, cohort study that was conducted on patients presenting with STEMI undergoing primary PCI. Patients age ≥ 18 years who presented within 12 hours after the onset of symptoms and who had ST-segment elevation ≥ 1 mm in ≥ 2 contiguous leads.
Posterior myocardial infarction (MI) was considered in presence of ST-segment depression ≥ 0.5 and tall R waves (Q wave equivalent) in V1-V3. These findings were confirmed by the presence of ST elevation and Q waves in the posterior leads (V7-9).
Exclusion criteria:
1. Patients with uninterpretable presenting ECG (paced rhythm, missing ECG or left bundle branch block);
2. Pseudo-q wave (E.g., Left Ventricular Hypertrophy);
3. History of prior MI;
4. History of prior revascularization (PCI or Coronary artery bypass graft).
A written informed consent was obtained from all eligible patients. This study was approved by Kasr al Ainy Ethics Committee in accordance with Declaration of Helsinki.
Baseline variables
All patients were evaluated by clinical assessment, laboratory tests (including cardiac enzymes), echocardiography at baseline, and on discharge.
For all eligible patients, detailed history and clinical examination was performed with special emphasis on:
1.Risk factors for cardiovascular diseases.
-Hypertension: It was defined as elevation of arterial systolic blood pressure (SBP) ≥ 140 mmHg and/or diastolic blood pressure (DBP) ≥ 90 mmHg on two or more properly measured seated blood pressure readings on two or more office visits or patients who were taking anti-hypertensive medications (9).
-Diabetes mellitus (DM): It was defined as 8 hours fasting plasma glucose ≥ 6.99 mmol/l, 2-h plasma glucose ≥ 11.1 mmol/l during an oral glucose tolerance test, symptoms of DM and casual plasma glucose ≥ 11.1 mmol/l or patients who were taking anti-diabetic medications (10).
-Dyslipidemia: It was defined as total cholesterol > 11.1 mmol/l or low-density lipoprotein - cholesterol (LDL-C) ≥ 7.21 mmol/l (11). Complete lipid profile was obtained after admission (12).
-Current smoking: Current smoking was defined as smoking within one month of recruitment.
-Peripheral vascular disease: History of chronic lower limb threatening ischemia, previous acute limb ischemia, previous peripheral revascularization.
-Cerebrovascular accident: Previous stroke, transient ischemic attacks.
2.Heart rate (HR), systolic blood pressure, diastolic blood pressure (in supine position).
3.Current medications if the patient was kept on medical treatment.
ECG analysis
All patients underwent 12-lead ECG recordings. The definition of Q waves was based on the earlier definition of pathological Q wave defined as wave with more than 0.04s of duration and with an amplitude of more than 25% of the corresponding R-wave (2-4).
In this study, presenting ECGs were analyzed for presence or absence of Q waves and correlated with different clinical predictors and angiographic findings.
Coronary angiography data
For all eligible patients, Adequate pre-procedure and post-procedure angiographic data were obtained with special emphasis on:
-Symptom to balloon time (STB) were calculated for all patients.
-Coronary angiography and PCI were done through the femoral or radial approach.
-All patients received the following regimen: (1) Clopidogrel 600 mg initial dose followed by a maintenance dose of 75 mg once daily or ticagrelor 180 mg loading dose orally followed by a maintenance dose of 90 mg twice daily (2); aspirin 300 mg followed by 75 – 100 mg/day; (3) During the procedure patients received unfractionated heparin (70-100 IU/kg).
-Diagnosis of culprit coronary artery: Left main vessel, left anterior descending coronary artery, left circumflex coronary artery, obtuse marginal, right coronary artery, posterior descending coronary artery, and posterolateral branch involvement.
-Need of glycoprotein IIb/IIIa inhibitor (eptifibatide): in cases of slow flow, no reflow, heavy thrombus burden.
-Obstructive coronary artery disease was defined as a ≥ 50% stenosis in the coronary artery lumen.
Angiographic outcome
Thrombus burden (TB) was graded (G) as G0 = no thrombus, G1 = possible thrombus, G2 = small [greatest dimension ≤ 1/2 vessel diameter (VD)], G3 = moderate (> 1/2 but < 2VD), G4 = large (≥ 2VD), G5 = unable to assess TB due to vessel occlusion. In patients with G5 thrombus, burden score was calculated after passage of wire or small non-inflated balloon through the lesion (13). Thrombolysis in myocardial infarction (TIMI) flow rate was assessed at the end PPCI (14).
No-reflow was defined as inadequate myocardial perfusion through a given segment of the coronary circulation without angiographic evidence of mechanical vessel obstruction (15).
Statistical analysis
Sample size calculation
Based on previous studies and clinical experience, we predicted proportions of occurrence of the primary variables. For a desired power of 0.85 and a Type I error rate of 0.05, we enrolled 260 participants.
We used for sample size calculation (OpenEpi: Open-Source Epidemiologic Statistics for Public Health, Version 3.01. www.OpenEpi.com, updated 06/04/2013).
Data analysis was performed using the SPSS 25.0 statistical package for Windows (SPSS Inc., Chicago, Ill, USA).Continuous variables, reported as the mean and standard deviation and were compared using a 2-sample Wilcoxon rank sum test. Categorical variables, reported as a percentage of the total, were compared using a Pearson Chi-square tests.
To determine which patient characteristics were correlated with Q waves, odds ratios (ORs) were calculated. A multivariate logistic regression model was performed including baseline characteristics to determine which variables are independently associated with Q wave development.
A logistic regression model was performed to determine the association between Q waves and different angiographic findings and another model was performed to determine association between different baseline characteristics and different angiographic findings.
A p-value < 0.05 was regarded as statistically significant.
Results
Three hundred and seventeen STEMI patients were enrolled. Two hundred and sixty-two patients were eventually included in the study as shown in Figure 1.
The mean age of patients was 54 (10) years. Eighty four percent of the recruited patients were males. Dyslipidemia represents the most common risk factor among half of the study patient population.
Baseline patients characteristics and correlates of Q wave development
A total of 121 patients (41%) had a Q wave identified among 262 recruited patients. Table 1 summarized baseline patients characteristics stratified by the presence of Q waves. Both dyslipidemia and time from symptoms onset were independently and positively correlated with the presence of a Q wave (adjusted OR: 1.8, 95% confidence interval [CI]: 1.09 – 2.7, P = 0.04 for dyslipidemia, (adjusted OR: 1.35 per 10 hrs, 95% CI: 1.09-1.67, P = 0.002). Patients with Q waves were more likely to have higher heart rate compared to STEMI patients without pathological Q waves (p= 0.003). Other variables as age, Gender, Hypertension, prior cerebrovascular accident, and systolic blood pressure were not statistically different between both patient groups.
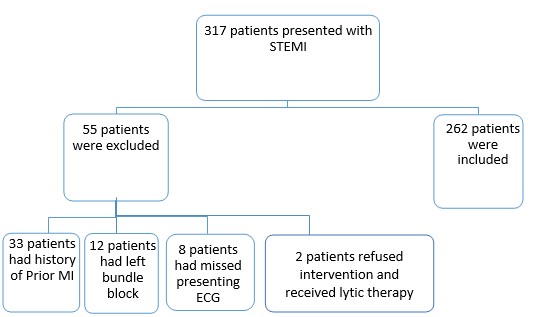
Figure 1. Diagram of enrolled patients
|
Table 1. Baseline characteristics of patients stratified by the presence of Q waves |
|||
|
Variables |
Q wave (n = 121) |
No Q wave (n = 141) |
p |
|
Age, years |
55 (11) |
54 (10) |
0.27 |
|
Male gender, n (%) |
97 (80) |
120 (85) |
0.29 |
|
Diabetes, n (%) |
41 (34) |
51 (36) |
0.69 |
|
Hypertension, n (%) |
47 (39) |
43 (30) |
0.92 |
|
Current smokers, n (%) |
106 (87) |
88 (62) |
0.65 |
|
Dyslipidemia, n (%) |
72 (60) |
67 (46) |
0.04 |
|
Previous stroke, n (%) |
5 (4) |
7 (5) |
0.74 |
|
Chronic kidney disease, n (%) |
3 (2) |
4 (3) |
0.85 |
|
Time from symptoms onset to Intervention, hours |
10 (4) |
7 (3) |
0.002 |
|
Door to balloon time, minutes |
92 (33) |
90 (38) |
0.38 |
|
Systolic blood pressure, mmHg |
131 (27) |
133 (30) |
0.66 |
|
Heart rate, beats/minute |
89 (18) |
80 (18) |
0.003 |
|
Data are presented as mean (standard deviation) or number (% of total) |
|||
Angiographic findings and their association with Q wave development
Angiographic characteristics stratified by Q wave are shown in Table 2. Patients with Q waves were more likely to have thrombus grade III - IV at the time of angiography (adjusted OR: 1.4, p = 0.009), more likely to have TIMI flow grade < III (adjusted OR: 0.89, p = 0.04) after primary PCI. There is no statistical difference between both patients’ groups regarding no reflow phenomena (adjusted OR: 1.27, p = 0.45).
|
Table 2. Angiographic characteristics stratified by the presence of Q waves |
||||
|
Angiographic outcome |
Q wave (%) |
No Q wave (%) |
Adjusted OR (95% CI) |
p |
|
TIMI < III flow |
115/121 (95) |
112/141 (79) |
0.89 (0.81 – 0.98) |
0.04 |
|
Thrombus grade III – IV |
118/121 (97) |
89/141 (63) |
1.4 (1.10 – 1.60) |
0.009 |
|
NO Reflow |
25/121 (21) |
24/141 (17) |
1.27 (0.68 – 2.36) |
0.45 |
|
CI - confidence interval, OR - odds ratio, TIMI - Thrombolysis in Myocardial Infarction |
||||
Baseline patient characteristics and association with different angiographic results
Dyslipidemia was independently and positively correlated with no reflow phenomena in STEMI patients who had undergone primary PCI strategy ( p = 0.03).
Diabetes and time from symptoms onset to intervention were independently and positively correlated with presence of thrombus grade III - IV after PCI (P = 0.007 and 0.003, respectively).
Age, diabetes, and hypertension were independently and positively correlated with low myocardial perfusion grade (TIMI flow < 3) during angiography (p = 0.03, 0.02, 0.04, 0.01, respectively).
Discussion
Association between clinical risk factors and Q waves in STEMI patients
We found that dyslipidemia and time from symptom onset to intervention were independent predictors for development of Q waves (adjusted OR: 1.8, 95% CI: 1.09 – 2.7, p = 0.04 for dyslipidemia, (OR: 1.35 per 10 hours, 95% CI: 1.09-1.67, p = 0.002 for time from symptom onset to intervention).
In contrast to our study, in the GRACE (Global Registry of Acute Coronary Events) registry that included 3929 patients, a multivariate analysis showed that presenting Q-waves were associated with male sex (OR 1.28), increased age (OR 1.06 per 5 years), diabetes (OR 1.26), smoking (OR 1.11), chronic aspirin (OR 0.79) and acute aspirin (OR 0.87) use. Different results can be explained by difference in sample size and that our study was a prospective cohort one in contrast to GRACE registry , which was a multicenter observational cross-sectional study (16).
Prognostic significance of the Q-wave development
Patients with Q waves were more likely to have severe thrombus burden at the time of angiography (OR: 0.4, p=0.009), more likely to have TIMI flow grade < III (adjusted OR: 0.89, p=0.04). Similar results were shown in several studies. In Subgroup analysis of Hirulog Early Reperfusion/Occlusion (HERO-1) trial recruiting 362-patients, Q waves on the presenting ECG were associated with lower rates of TIMI 3 flow (35% vs 55%, p< 0.001) (17).
Similarly, In the GRACE registry, the presence of Q waves was associated with significantly reduced infract-related artery flow from larger thrombus burden (16).
Correlation between Q waves and reduced TIMI flow has also been observed in patients treated with facilitated and primary PCI and these studies concluded that the development of Q waves was associated with large thrombus and more extensive obstruction to coronary blood flow. All these prevent successful reperfusion therapy (7, 18).
Observations from the CLARITY trial that recruited 3491 STEMI patients treated with fibrinolysis, Q waves were associated with lower rates of reperfusion as assessed by complete ST resolution, normal TIMI flow, and normal TIMI myocardial perfusion grade after fibrinolysis, However, in this study, fibrinolysis was used as the intervention method for all STEMI incomers, while primary PCI was used in our study (19).
Association between clinical risk factors and angiographic findings
In our study, we analyzed associations between different baseline characteristics and angiographic findings in STEMI patients. Dyslipidemia was considered an independent predictor of no reflow (p=0.03).
While diabetes and time from symptoms onset to intervention were considered independent predictors for presence of thrombus (p=0.007 and p=0.003, respectively). Age, diabetes, and hypertension were considered independent predictors for low myocardial perfusion grade (TIMI flow < III).
Similar to our study, Mazhar et al. concluded that no-reflow during primary PCI was more likely with older age and delayed presentation (20).
In contrast to our study, Ge et al. (21) studied the determinants of angiographic thrombus burden in 182 young patients with STEMI and concluded that hypertension is an independent determinant of high thrombus burden compared to patients with low thrombus burden (p<0.001). However, the latter study compared STEMI patients with heavy and low thrombus burden (21). In our study, we addressed independent predictors for presence of thrombus regardless of severity.
Possible therapeutic improvement
In our study, we addressed several logistic issues that need improvement.
1. To shorten logistic time of admission of patients from emergency department to catheterization laboratory.
2. To facilitate availability of aspiration catheters that will help to decrease incidence of no reflow phenomena.
Study limitations
1.Being a single-center observational study with a relatively small patient cohort number, both were considered a limitation of this study.
2.Assessment of myocardial blush grade was not performed as several angiogram films were not acquired long enough to visualize the myocardial blush.
Conclusion
Among STEMI patients, both dyslipidemia and time from symptoms onset to intervention were independent predictors for development of Q waves. The presence of Q waves was strongly associated with heavy thrombus burden at time of intervention and TIMI flow grade < III after primary PCI.
Ethics: Informed consent was obtained from all patients included in the study. This study was approved by Kasr al Ainy Ethics Committee in accordance with Declaration of Helsinki.
Peer-review: External and internal
Conflict of interest: None to declare
Authorship: A.Y.H., T.A.H., M.A.R., and H.H.K. equally contributed to the study and preparation of manuscript, fulfilled authorship criteria
Acknowledgement: We acknowledge all our residents, fellows and nursing staff whom supported this work and without whom this study wouldn’t have been completed
Funding: None to declare
Statement on A.I.-assisted technologies use: Authors declare that they did not use AI-assisted technologies in preparation of this manuscript
Availability of data and material: Data supporting our findings are available and will be made available on reasonable request. Fair use in frame of ethics with acknowledgement of authors and source, is required.
References
| 1. Delewi R, IJff G, van de Hoef TP, Hirsh A, Robbers LF, Njveldt R, et al. Pathological Q waves in myocardial infarction in patients treated by primary PCI. JACC: Cardiovasc Imag 2013; 6: 324-31. doi: 10.1016/j.jcmg.2012.08.018 https://doi.org/10.1016/j.jcmg.2012.08.018 PMid:23433932 |
||||
| 2. Krone RJ, Friedman E, Thanavaro S, Miller JP, Kleiger RE, Oliver GC. Long-term prognosis after first Q-wave (transmural) or non-Q-wave (nontransmural) myocardial infarction: analysis of 593 patients. Am J Cardiol 1983; 52:234-9. doi:10.1016/0002-9149(83)90114-5 https://doi.org/10.1016/0002-9149(83)90114-5 PMid:6869266 |
||||
| 3. Maisel AS, Ahnve ST, Gilpin EL, Mueller C, Neath SX, Christenson RH, et al. Prognosis after extension of myocardial infarct: the role of Q wave or non-Q wave infarction. Circulation 1985; 71: 211-7. Doi: 10.1161/01.CIR.71.2.211 https://doi.org/10.1161/01.CIR.71.2.211 PMid:3965166 |
||||
| 4. Williams RA, Cohn PF, Vokonas PS, Young E, Herman MV, Gorlin R. et al. Electrocardiographic, arteriographic and ventriculographic correlations in transmural myocardial infarction. Am J Cardiol 1973; 31: 595-9. Doi: 10.1016/0002-9149(73)90328-7 https://doi.org/10.1016/0002-9149(73)90328-7 PMid:4698129 |
||||
| 5. Thygesen K, Alpert JS, White HD, Chaitman BR, Bax JJ, Morrow DA, Whiter HD, et al. Fourth universal definition of myocardial infarction. Expert consensus document. Circulation 2007; 116: 2634-53. Doi: 10.1161/CIRCULATIONAHA.107.187397 https://doi.org/10.1161/CIRCULATIONAHA.107.187397 PMid:17951284 |
||||
| 6. Siha H, Das D, Fu Y, Zheng Y, Westerhout CM, Storey RF.,et al. Baseline Q waves as a prognostic modulator in patients with ST-segment elevation: insights from the PLATO trial. CMAJ 2012; 184: 1135-42. Doi: 10.1503/cmaj.111683 https://doi.org/10.1503/cmaj.111683 PMid:22546885 PMCid:PMC3394819 |
||||
| 7. Armstrong PW, Fu Y, Westerhout CM, Hudson MP, Mahaffey KW, White HD, et al. Baseline Q-wave surpasses time from symptom onset as a prognostic marker in ST-segment elevation myocardial infarction patients treated with primary percutaneous coronary intervention. J Am Coll Cardiol 2009; 53: 1503-9. doi:10.1016/j.jacc.2009.01.046 https://doi.org/10.1016/j.jacc.2009.01.046 PMid:19389560 |
||||
| 8. Wong CK, Gao W, Raffel OC, French JK, Stewart RA, White HD: HERO-2 Investigators. Initial Q waves accompanying ST-segment elevation at presentation of acute myocardial infarction and 30-day mortality in patients given streptokinase therapy: an analysis from HERO-2. Lancet 2006; 367: 2061-7. Doi: 10.1016/S0140-6736(06)68929-0 https://doi.org/10.1016/S0140-6736(06)68929-0 PMid:16798389 |
||||
| 9. Ram CV, Giles TD. The evolving definition of systemic arterial hypertension. Curr Atheroscler Rep 2010; 12: 155-8. doi: 10.1007/s11883-010-0107-6 https://doi.org/10.1007/s11883-010-0107-6 PMid:20425253 |
||||
| 11. American Diabetes Association. Diagnosis and classification of diabetes mellitus. Diabet Care 2010; 33(Supplement_1): S62-9. doi:10.2337/dc13-S067. https://doi.org/10.2337/dc13-S067 PMid:23264425 PMCid:PMC3537273 |
||||
| 10. Jeong SM, Choi S, Kim K, Kim SM, Lee G, Park SY,et al. Effect of change in total cholesterol levels on cardiovascular disease among young adults. J Am Heart Assoc 2018; 7: e008819. Doi: 10.1161/jaha.118.008819 https://doi.org/10.1161/JAHA.118.008819 PMid:29899019 PMCid:PMC6220545 |
||||
| 12. Sidhu D, Naugler C. Fasting time and lipid levels in a community-based population: a cross-sectional study. Arch Int Med 2012; 172: 1707-10. doi:10.1001/archinternmed.2012.3708 https://doi.org/10.1001/archinternmed.2012.3708 PMid:23147400 |
||||
| 13. Gibson CM, de Lemos JA, Murphy SA, Marble SJ, McCabe CH, Cannon CP, Antman EM, et al. Combination therapy with abciximab reduces angiographically evident thrombus in acute myocardial infarction: a TIMI 14 substudy. Circulation.2001; 103: 2550-4. doi:10.1161/01.CIR.103.21.2550 https://doi.org/10.1161/01.CIR.103.21.2550 PMid:11382722 |
||||
| 14. Gibson CM, Ryan KA, Kelley M, Mesley R, Murphy S, Swanson J, et al. Methodologic drift in the assessment of TIMI grade 3 flow and its implications with respect to the reporting of angiographic trial results. Am Heart J 1999; 137: 1179-84. doi: 10.1016/S0002-8703(99)70380-7 https://doi.org/10.1016/S0002-8703(99)70380-7 PMid:10347349 |
||||
| 15. Kloner RA, Ganote CE, Jennings RB. The no-reflow phenomenon after temporary coronary occlusion in the dog. J Clin Invest 1974; 54: 1496-508. doi: 10.1172/JCI107898 https://doi.org/10.1172/JCI107898 PMid:4140198 PMCid:PMC301706 |
||||
| 16. LaBounty T, Gurm HS, Goodman SG, Montalescot G, Lopez-Sendon J, Quill A, Eagle KA. GRACE Investigators. Predictors and implications of Q-waves in ST-elevation acute coronary syndromes. Am J Med 2009; 122: 144-51. Doi: 10.1016/j.amjmed.2008.08.029 https://doi.org/10.1016/j.amjmed.2008.08.029 PMid:19185091 |
||||
| 17. Wong CK, French JK, Aylward PE, Frey MJ, Adgey AA, White HD. Usefulness of the presenting electrocardiogram in predicting successful reperfusion with streptokinase in acute myocardial infarction. Am J Cardiol 1999; 83: 164-8. https://doi.org/10.1016/S0002-9149(98)00818-2 PMid:10073815 |
||||
| Doi:10.1016/S0002-9149(98)00818-2 https://doi.org/10.1016/S0002-9149(98)00818-2 PMid:10073815 |
||||
| 18. McDonald MA , Fu Y, Zeymer U, Wagner G, Goodman SG, Ross A, et al. Adverse outcomes in fibrinolytic-based facilitated percutaneous coronary intervention: insights from the ASSENT-4 PCI electrocardiographic substudy. Eur Heart J 2008; 29: 871-9. Doi: 10.1093/eurheartj/ehn078 https://doi.org/10.1093/eurheartj/ehn078 PMid:18319519 |
||||
| 19. Waks JW, Sabatine MS, Cannon CP, Morrow DA, Gibson CM, Wiviott SD, et al. Clinical implications and correlates of Q waves in patients with ST‐elevation myocardial infarction treated with fibrinolysis: Observations from the CLARITY‐TIMI 28 Trial. Clin Cardiol 2014; 37: 160-6. Doi: 10.1002/clc.22235 https://doi.org/10.1002/clc.22235 PMid:24452727 PMCid:PMC6649643 |
||||
| 20. Mazhar J, Mashicharan M, Farshid A. Predictors and outcome of no-reflow post primary percutaneous coronary intervention for ST elevation myocardial infarction. IJC Heart & Vasc 2016; 10: 8-12. doi: 10.1016/j.ijcha.2015.11.002 https://doi.org/10.1016/j.ijcha.2015.11.002 PMid:28616509 PMCid:PMC5441318 |
||||
| 21. Ge J, Li J, Dong B, Ning X, Hou B. Determinants of angiographic thrombus burden and impact of thrombus aspiration on outcome in young patients with ST‐segment elevation myocardial infarction. Cathet Cardiovasc Interv 2019; 93: E269-76. Doi: 10.1002/ccd.27944 https://doi.org/10.1002/ccd.27944 |
||||
Copyright

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.
AUTHOR'S CORNER

